How to Protect Your Baby in the ICU
By Elisabeth Snell
Printed in Practical Homeschooling #96, 2010.
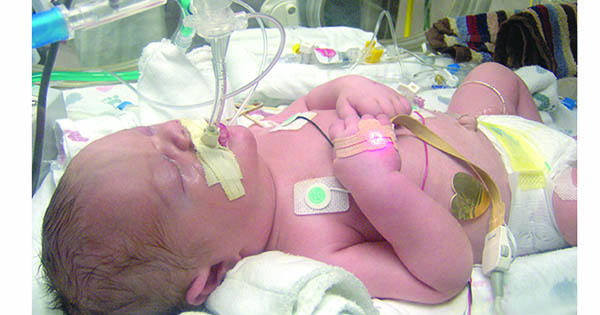 If you should ever have a child or grandchild in the ICU, here's good advice to help the little one survive the experience.
If you should ever have a child or grandchild in the ICU, here's good advice to help the little one survive the experience.

| 
|
INTRODUCTORY NOTE from Mary Pride, Editor of PHS: We realize that this
is not, strictly speaking, a “homeschooling” article. However, as the
mother of a NICU baby myself, I instantly realized what a godsend this
article would be to anyone in this position. I urge you to save this
article in case you, a family member, a neighbor, or a friend end up
needing its advice.

I am the mother of an heart/lung bypass baby. In the time we had to
spend in NICU (Newborn Intensive Care Unit) and ICU (Intensive Care
Unit) we learned some things the hard way. I wish I’d had this list
beforehand.
1 Whatever your baby’s condition, it will become much worse quickly
if they catch a virus or bacterial infection which is very likely
while in the hospital. You must be fearsome in protecting your child
from unwashed contact. Doctors, nurses, surgeons on follow-up: ANYONE
who enters your room must be asked to sanitize their hands in front of
you. Post a sign that says “Please wash your hands before touching
me.” Hospitals encourage insisting on washed hands, but often in
practice you’ll sense frustration when you ask a doctor or nurse to
sanitize again. They’ll often say “I just did outside the door,” but
then they touched your door handle, which is a germ pit. Or they enter
wearing gloves which might have been used on other patients, or at the
least have touched your door. Often doctors and nurses think of gloves
as protecting themselves, and don’t automatically think about the
patient. After they’re sanitized, watch for:
- Answering a cell phone call. Studies have shown this is a major
way illness spreads. Pretend all cell phones belonging to anyone in
your room have just come from a horrible disease-filled room, because
they probably have.
- Touching handles of drawers, light switches, faucets—anything
like that is a germ touchpoint.
- Touching their face (especially the nose) or their hair.
- Instruments: be certain they sterilize the stethoscope, sonogram,
blood pressure cuff, anything they move from patient to patient.
- If they come in isolation gear (gown, mask, gloves or any
component of these things) and your child isn’t in isolation—LOOK OUT.
They’ve just come from a room where someone is confirmed with a viral
or bacterial infection. Even if your child has an infection already,
the child down the hall probably has a different one.
- If anyone appears to be ill or having “bad allergies” beware.
Most illnesses are contagious a day or so before the first symptoms
show.
- Limit people coming right after being in a store or crowd. Their
clothes are so germy.
- If someone goes out of the room and right back in after fetching
a blanket or something, they must resanitize.
- If anything falls on the shiny hospital floor, pretend it fell
into a toilet because a hospital floor is worse. There’s blood, pus,
feces, etc. all over the floor because the bottoms of shoes are
carrying it in from room to room.
2 Ask questions. What is that medication? Why does my baby need it?
Will it interfere with my baby’s heart rate/breathing/whatever your
crisis is. Many deaths occur because the wrong medication (or the
wrong amount) is given to a child. This is especially important if you
have new staff on duty.
3 Keep everyone up to date on your child’s sensitivities. If you know
your child is allergic or has a bad response to something (whether
drug, shampoo, adhesive, whatever), post it in LARGE LETTERS on their
bed in a prominent place. Don’t assume everyone knows because it’s in
the chart. Be vocal about these things, because every new doctor or
nurse will go back to the default drugs or treatment for the condition
unless they are aware your child is sensitive. They don’t have time to
read every patient’s chart from cover to cover before treating. Also,
the little shampoo rashes and things are important to note because
they can lead to the child being treated improperly for infection.
4 If you look at the swine flu deaths you’ll see a spike in deaths
every weekend. There’s often a transition in staff, and they don’t
know the child as well. If you have to be there over the weekend, keep
someone who knows the baby there overnight.
5 Every time the doctors rotate (usually every two weeks) you need to
meet the new doctor and give them history, allergies, any special
things. Explain why you don’t use drug x, or why this normal treatment
didn’t work well in the past. A lot of these things don’t get passed
along.
6 If a doctor is, in your opinion, making poor choices for your child
and will not listen to you, go to the floor supervisor and request a
different doctor from a different team. This will not affect your
nurses, usually. This does happen. The doctor may (probably will) come
and try to pressure you, so make sure you have someone with you. We
had many, many wonderful doctors, and one who wanted to experiment on
our child with his own private theories of treatment instead of going
the traditional route. When we argued because of the deterioration of
our child’s condition, he came to “listen” but really just tried to
sell us again on his course of treatment and admonished us for taking
time out of his rounds every day. So we relieved him of the hassle of
working with us, and were much happier with Doctor #2. After the fact,
we learned other medical staff had thought his decisions were rash,
but no one came and told us until we stepped up and insisted on a
different doctor.
7 Go with your gut. While in the ICU we met a young mother who had a
baby she thought from the beginning was very ill. She asked the doctor
to transport the baby to the area hospital with the highest level ICU.
The doctor argued with her and said she was a first-time mom and was
being overprotective. Nevertheless, she insisted, but when the doctor
called the other hospital for transport, he told them the baby was
fine and it was just an anxious mother. So, the transport team took
their time getting there and were furious to find the baby had
declined so much that she was too unstable to transport. They had to
work on stabilizing her for four hours before they could even move
her. She was a very, very sick little baby and mom was right. Don’t
worry about people thinking you’re crazy—you know this baby better
than anyone else, and you are probably right. If no one will listen to
you, call guest relations and ask for an advocate. Ask for a social
worker to help you.
8 If teams of nurses are touring through to show off your baby’s
high-tech equipment to other nurses and say things like, “We hardly
ever have to use this,” or, “In my time working here I’ve only seen
three babies on this,” odds are good you are in the wrong hospital for
your baby’s condition and should get out NOW. If your hospital is
consulting with other doctors at a larger hospital to figure out
treatments, go to the larger hospital. Don’t worry that it’s far or
that you don’t know how to get there. Usually the big hospitals are
much more equipped for longer ICU stays and have things like showers
for the families, beds to sleep in the room, a much smaller
nurse-to-patient ratio, and more knowledge on treatments for your
baby.
9 Don’t wait until things are going down to transport. If the baby
may need more equipment, transport when the baby’s stable. Otherwise
they sometimes die in transport. As the mom of a baby who required the
very most life support you can receive, I was very thankful for this
advice. I think it probably helped save my baby’s life.
10 Bring little snacks or gifts for your nurses and doctors. If you
have other children post their pictures in the room. Make little signs
for the baby. Bring in cute blankets. Whatever you can do to make it
more obvious your baby is a person and not a very sick project, the
more attention the child will likely get.
11 Do bond with your baby. Try to enjoy the little moments of
happiness in the middle of all of this. DO TAKE PICTURES. If your baby
heals up perfectly you’re going to want a chronicle of this terrible
walk. If your baby doesn’t get better, you will treasure every single
picture you have, tubes or not.
12 Sing to your baby, touch your baby—even if he or she appears to be
unconscious. This matters. Often babies are given a paralytic to keep
them from tearing out the tubes, but though they appear asleep because
they can’t move, they can hear and feel. Ask for music therapy if the
hospital has it.
13 Make eye contact as often as possible. Nurses are often doing
something else while handling your baby and can’t make eye contact.
Eventually after this “neglect” a baby will stop making eye contact
when people talk. Combat this by touching and eye contact as much as
possible. If your baby is “low stimulation” find out why and see if
it’s actually helping. If the answer is, “Oh because all of the babies
in this area are,” advocate for more skin contact.
14 Try to protect the baby’s sleep as much as possible. Being
constantly disturbed can make a baby frantic and jumpy. Try to set
aside some hours after a narcotic dose to let the baby sleep without
disruption.
15 Wear a washcloth in your shirt without any perfume or lotions.
Sleep in it, then leave it in the baby’s bed or cover baby’s eyes with
it so your scent is with him. This seems to improve healing.
16 It’s OK to grieve. You don’t have to put up a brave front for
everyone. It hurts to see your poor baby in tubes and drugs.
17 It’s OK to pray. We certainly did!
18 It’s OK to hope. Remember, you’re not the first parents to ever go
through this. Other families have found the strength to handle this
terrifying time, and you will, too.